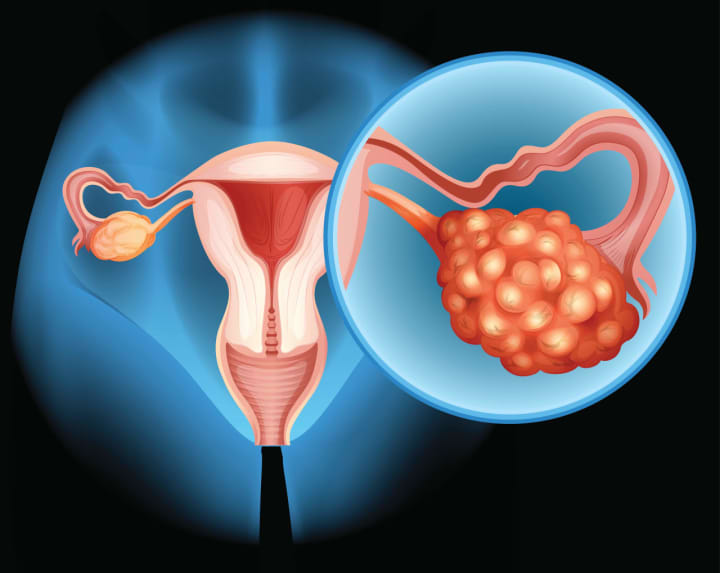
At one time or another, almost every woman will experience some of the symptoms of ovarian cancer, such as bloating, pelvic or abdominal pain, indigestion, decreased appetite, feeling full quickly or changes in urinary or bowel pattern. However, it is the persistence of these symptoms that should lead to consideration of the diagnosis of ovarian cancer, and result in careful evaluation of that possibility.
Although ovarian cancer can strike women of any age, the disease is more likely to occur in postmenopausal women over age 55. Women are at an increased risk of ovarian cancer if they have a genetic mutation such as BRCA 1 or BRCA 2, a family history of breast or ovarian cancer, Lynch syndrome (HNPCC, hereditary nonpolyposis colorectal cancer) or a personal history of other related cancers. A carefully conducted family history and genetic counseling can help determine a woman’s individual risk for the disease.
While there is no consistently reliable screening test for ovarian cancer, women who are at risk or have symptoms of the disease may undergo testing such as a pelvic exam, a transvaginal ultrasound or a CA-125 blood test that detects a protein produced by the cancer. However, the only definitive test for ovarian cancer is a biopsy.
The good news is that the likelihood of surviving the disease is increased when ovarian cancer is treated at an early stage. When the cancer is confined to the ovaries, surgery can result in a cure rate greater than 90 percent.
Recent advancements in the treatment of ovarian cancer, including chemotherapy combinations and methods of delivery, immunotherapy and even additional surgery, are improving the quality and length of life of women with advanced ovarian cancer. In fact, ovarian cancer is often characterized as a chronic disease because more women are living with this cancer for a longer period of time than ever before.
If you are at risk for ovarian cancer or have been diagnosed with the disease, it is important to be treated at a comprehensive cancer center by a team of ovarian cancer gynecologic oncologists and specialty trained experts. The cancer center team should offer a full range of supportive services, including patient navigation for coordinated care, nutritional and psychosocial support, palliative care for symptom management -- as well as physical rehabilitation and survivorship clinics.
NewYork-Presbyterian Cancer Centers provide high-quality, comprehensive cancer care at convenient locations throughout the New York metropolitan area, Westchester and the Lower Hudson Valley in state-of-the-art, comfortable environments. Board certified oncologists collaborate with a multidisciplinary team of specialists to provide each patient with an individualized plan of care. To find a location in your area visit nyp.org/cancerlocations.
NewYork-Presbyterian is one of the largest and most comprehensive hospitals in the nation, ranked New York’s No. 1 hospital for the 16th consecutive year, and No. 6 in the United States, according to U.S. News and World Report. Affiliated with two academic medical colleges – Weill Cornell Medicine and Columbia University College of Physicians and Surgeons, NewYork-Presbyterian brings together internationally recognized researchers and clinicians to develop and implement the latest approaches for prevention, diagnosis and treatment. The Herbert Irving Comprehensive Cancer Center at NewYork-Presbyterian/Columbia University Medical Center is one of only three NCI-designated comprehensive cancer centers in New York State. NewYork-Presbyterian provides comprehensive cancer care at all of our locations across the New York Metro area including Westchester County and the Hudson Valley. Learn more at nyp.org/cancer.